Science applied to practice – Dr Kunal Shah and and Dr Asmaa Al-Taie
Featured Products Promotional FeaturesPosted by: Dental Design 15th August 2019

Dr Kunal Shah, Principal of LeoDental in London, and Dr Asmaa Al-Taie, Clinical Lecturer in Restorative Dentistry, Leeds, demonstrate the use of an amalgam alternative restorative in practice, as well as the science supporting the material.
Case presentation
A regular patient presented to the practice with pain from the ULQ localised to the UL6. She had a clear medical history and upon a full clinical assessment, no abnormalities were identified, she had good oral health and no TMJ issues. Following special tests, it was evident a carious lesion was present and so a restoration was indicated.
The choice needed to be made between an amalgam filling and a composite restoration. The patient voiced a preference for resin composite due to the improved aesthetics that could be achieved – the restoration was in the smile line.
The full treatment procedure was explained to the patient, who was happy to proceed and provided informed consent.
During the treatment, cavity preparation was undertaken to clean out any residual material and double check there were no caries. The tooth was then washed and dried and moisture control was obtained. Local anaesthetic was administered and a band and wedge placed. Scotchbond Universal adhesive self-etch from 3M Oral Care was applied in a single layer – as per the manufacturer’s instructions – and then light cured using the 3M Elipar Deepcure-S.
The restoration was built up in incremental layers using Filtek One bulk fill restorative from 3M. I would typically build the lateral wall first to ensure a good contact point, which I did in this case. I then removed the wedge and band completely, so there was effectively just an occlusal restoration left, which was built up cusp by cusp.
Once completed, the occlusion was checked with articulating paper in both occulsion and at rest, so that any high spots could be adjusted. The restoration was then dual polished and completed using finishing burs followed by green and white stones, to get a really good finish.
The science
Following the introduction of the Minimata Convention and the calls for reducing use of dental amalgam, dental composite remains the most suitable alternative as a direct posterior restorative material. However, unlike amalgam, conventional composites are light activated materials which require incremental build ups due to their limited depth of cure (Shortall, Palin and Burtscher, 2008)and to potentially reduce the consequences of shrinkage stress (Park et al., 2008). Consequently, composite placement is considered time consuming and technique sensitive. Accordingly, a new class of resin “bulk fill” composites have recently been introduced to enable restoration build-up in thick layers of up to 4 mm. The main advancements of bulk fill composite materials are related to the increased depth of cure, which probably relate to their higher translucency (Lassila et al., 2012)and low shrinkage stress due to modifications in the filler content and/or the organic matrix.
However, these perceived improvements may not indicate the mechanical properties of the material. Some concerns have been raised regarding the inferior mechanical properties of bulk fill materials when compared to conventional resin composites (Garoushi et al., 2013)(Ilie, Rencz and Hickel, 2013). For example, it has been suggested that the reduced mechanical properties of resin composites are mainly related to the reduced filler content (Leprince et al., 2014). Other factors which may influence mechanical properties include the possible use of plastifying monomers to reduce shrinkage stress, which makes the materials more prone to softening, and the use of alternative photoinitiators (Leprince et al., 2014).
Generally, increasing the filler content results in enhanced mechanical properties and reduced polymerisation shrinkage of resin based composites (Jun et al., 2013; Shah and Stansbury, 2014; Randolph et al., 2016).It was identified that a filler content of 60% vol is necessary to achieve adequate mechanical properties (Lohbauer et al., 2006; Randolph et al., 2016).
Filtek One bulk fill restorative (3M Oral Care) has a unique chemistry that enables an increased depth of cure while maintaining increased opacity and, more importantly, higher filler content (76.5% by weight (58.4% by volume). The inspiration of this chemistry was based on the earlier work by Shortall (2008) who concluded that optimising the filler/resin refractive index mismatch provides increased curing depth and assists shade-matching (Shortall et al., 2008). This concept is utilised in Filtek One manufacturing and is referred to as “Smart Contrast Ratio Management”, whereby managing the interaction and the refractive index between the resin and the filler, the opacity of the composite can be increased without sacrificing the depth of cure. Therefore, unlike other bulk fill composites, the mechanical properties of Filtek One restorative may not be reduced.
Ensuring optimum light polymerisation of resin composite as another key parameter that may influence the mechanical strength and the longevity of resin composites (Ceballos et al., 2009). Light curing remains a critically sensitive step due to the various factors that may influence the efficiency of the light curing process. The main factors are related to the features of the light curing unit (LCU) and the operation technique used.
Effect of type of LED LCU
The LCU technical features (light intensity, wave length range, diameter of the tip) and the conditions of polymerisation (curing mode and exposure time) are key for optimum polymerisation (Rueggeberg et al., 1994b, Torno et al., 2008).
Light Irradiance
The light irradiance (mW/cm2) and the overall energy (mJ/cm2) are both essential to ensure optimum polymerisation. The overall energy required to cure resin composites is based on the below equation:
Energy (mJ/cm2) = Irradiance (mW/cm2) x Time (s)
The energy requirement to cure a 2mm composite increment was found to range between 16-24 J/cm2, giving a light irradiance of 16000-24000mJ/cm2 (Rueggeberg et al., 1994a). Based on this, curing a composite increment in 20 seconds would require a minimum irradiance of 800mW/cm2from the light source. Most manufactures suggest minimum irradiance requirements for their materials. Clinicians need to ensure that their LCUs are emitting light suitably and curing for the right amount of time based on the above equation.
Spectral output
To adequately cure a resin composite, the spectral output from the LCU must match the wavelength used by the photoinitiator in the resin. Most LED units emit light at a broad spectrum of wavelengths ranging from 375 to 510 nm. Therefore, most LCU units will efficiently cure resins containing camphorquinone (CQ), which is the most commonly used photoinitiator.
However, CQ is yellow in colour and this limits the amount that can be used in resin composites. Consequently, alternative photoinitiators have recently been introduced to overcome the issue, such as monoacylphosphine oxide (Lucirin TPO) and 1-Phenyl 1,2- Propanedione, which are activated by shorter wavelengths of 350-420 nm.
A suitable LED unit with two or more different wavelength ranges – like polywave LED LCUs – will therefore be required to ensure optimum polymerisation of resin composites containing such alternative photoinitiators. Polywave LED units produce a shorter violet wavelength and a longer blue wavelength. Violet light is used to activate photoinitiators that are sensitive to light within the range of 350–420 nm wavelength and blue light activates photoinitiators (mainly CQ) with maximum absorbance of light close to 468 nm. However, the homogeneity of the light output could be affected due to the different positions of each of the light emitters within the LED unit (Price et al., 2010b).
Light Beam Homogeneity
Analysis of the LCU tip shows that most units emit the light in a non-homogeneous way; some regions of the LCU emit high intensity light (hot spots), while other areas of the same LCU unit emit a lower irradiance of curing light (cold spots) (Price et al., 2011). Clinically, this may well impact the light distribution over large restorations with different mesiodistal and buccolingual dimensions. The effect of variable irradiance distribution has been shown to have a significant effect on the degree of conversion and surface microhardness of resin composites (Price et al., 2014, Haenel et al., 2015). Therefore, it is essential to ensure suitable choice of LED unit with homogenous light output. The cavity size should also be considered, as it may require overlapping of curing cycles to avoid different degrees of polymerisation within the restoration that could impact restoration longevity.
Operating technique
Another factor that may influence the light curing process is the operating method, including distance from the restoration, handling technique and barriers that may affect the overall irradiance of the unit. Therefore it is essential to ensure that clinicians are using the correct light curing protocol and employing a suitable unit that matches the composite material used.
Effect of distance from the restoration
Various clinical situations do not allow the light curing tip to be directly placed over the resin composites. The location and the depth of the cavity in posterior teeth affect the accessibility and the direction of the light beam which could limit the polymerisation of the resin composite due to reduced light output. A reduction in light output of 22% at a distance of 2 mm and 53% at 6 mm has been reported (Pires et al., 1993, Price et al., 2010a). Taking into consideration the average depth of a class II cavity (6 mm from tip of cusp to base of the box), the base of a class II composite restoration would then receive significantly less light irradiance.
Effect of barriers
Matrix bands, protective sleeves, ceramic materials and tooth layers (enamel/dentine) can act as barriers that significantly reduce the light irradiance and the total energy that reaches the resin composites. It was reported that the transmitted light output decreases by increasing the thickness of the barriers with a reduction of 53% when light is transmitted through 0.5 mm of composite or dentine (Price, Murphy and Derand, 2000). Consequently, it is recommended to double the curing time with an average of 1 mm of thickness of the barrier such as ceramics (AlShaafi, AlQahtani and Price, 2014).
Elipar Deepcure-S
Elipar Deepcure-S (3M Oral Care) was used in this clinical case with 1,200 mW/cm2light output. One of the unique features of this unit is the ability of the device to maintain sufficient light output to around 700 mW/cm2, which, at a 7 mm distance, allowed adequate curing of deep posterior restorations presented in this article. In addition to that, the 10 mm light guide illuminates up to 80% more curing surface compared to other models, allowing homogeneous polymerisation of large resin composite restorations.
Conclusion
Various factors have been identified to influence the light curing process and the polymerisation of resin composites, which ultimately may impact on the longevity of the composite restorations. Careful selection and maintenance of the LED unit in addition to careful handing is essential for a successful resin composite restoration.
Images
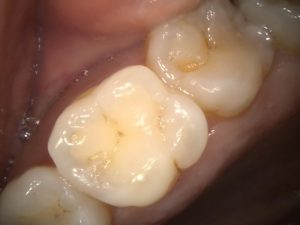
Figure 1 – Pre-op UL6
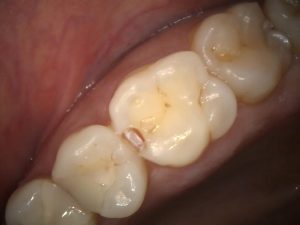
Figure 2 – Mid-Prep UL6 DO Cavity showing lesion
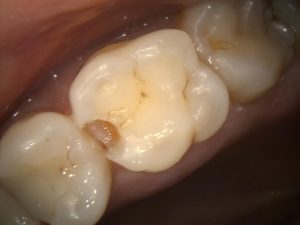
Figure 3 – Mid-prep UL6 DO cavity
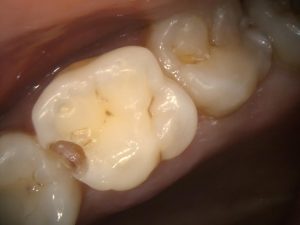
Figure 4 – Mid-prep UL6 DO cavity
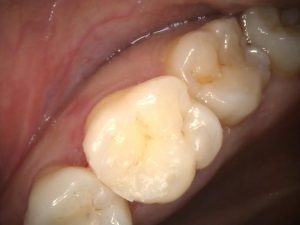
Figure 5 – UL6 DO Incremental Placement of Filtek Universal with excess Interproximally
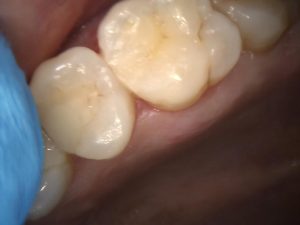
Figure 6 – UL6 DO Initial Placement of Filtek Universal with excess Interproximally
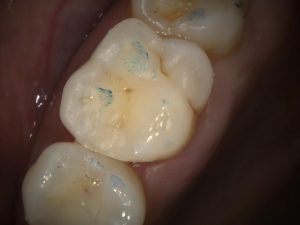
Figure 7 – UL6 DO Filtek Universal Bite Check and Polish

Figure 8 – UL6 DO Filtek Universal Bite Check
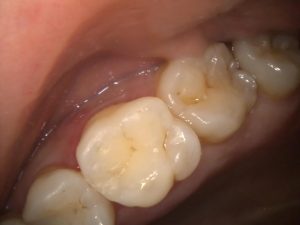
Figure 9 – UL6 DO Filtek Universal Final Polish
For more information, call 0800 626 578 or visit www.3M.co.uk/Dental
Authors:
 Kunal Shah is the Principal of LeoDental in London. He graduated from Birmingham, was selected as a Finalist for ‘Best Young Dentist South’ 2018 at The Dental Awards, and has the accolade for Best Implant and Imaging Clinic – London 2018.
Kunal Shah is the Principal of LeoDental in London. He graduated from Birmingham, was selected as a Finalist for ‘Best Young Dentist South’ 2018 at The Dental Awards, and has the accolade for Best Implant and Imaging Clinic – London 2018.
Having published several articles in the professional press and lectured
Internationally, he has a keen interest on the topics of digital dentistry, Implantology and restorative dentistry specific to direct resin composites and Impression materials. Dr Shah is also a clinical mentor for students on the year Long Postgraduate Implant Course at LeoDental in conjunction with SmileTube.tv.
referral@leodental.co.uk
 Dr Asmaa Al-Taie
Dr Asmaa Al-Taie
BDS, MSc, MFDS RCS (Ed), PhD
Asmaa is a Clinical Lecturer/Speciality Registrar in Restorative Dentistry at the Leeds Dental Hospital. She completed her MSc (distinction) and PhD at Leeds. She has also been awarded the Membership Diploma from the Faculty of Dental Surgeons, (Royal College of Surgeons of Edinburgh). For her PhD she developed novel nano-hybride dental composite with anticaries properties. Her research interests is in the field of resin composites, light curing and amalgam alternatives. She has an interest in rehabilitating tooth surface loss patients with direct resin composites and all aspects of fixed and removable prosthodontics. She published in the fields of dental composites, removable prosthodontics, endodontics and the rehabilitation of oral cancer patients. She has an interest in both undergraduate and postgraduate education and has lectured nationally and internationally.









