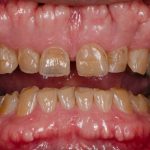
The UK soft drinks industry has a market value of £16 billion, with carbonated drinks the largest sector at 40%. As such, in 2021, the UK consumed 14,520 million litres of soft drinks, averaging at around 105 litres per person.[i] With this in mind, clinicians should consider the effects this may be having on their patients’ oral health, and the ways in which the nation’s fizzy drinks obsession may be contributing to tooth wear. Dental professionals must also acknowledge the ways in which acting early could help prevent severe tooth wear, tooth fracture, and tooth loss.
Causes of tooth wear
In order to understand the nature of tooth wear, it’s important to understand its potential causes. This enables clinicians to more effectively manage the problem and advise their patients appropriately. Usually caused by a combination of chemical and mechanical factors, tooth wear is the cumulative loss of tooth structure. It is a natural part of ageing, but those with severe tooth wear in their younger years should be treated accordingly as it can lead to poor aesthetics and affect the teeth’s lifespan.[ii]
Research suggests that increased tooth wear is associated with extrinsic acid from food, drinks, and medications, as well as intrinsic acids caused by gastro-oesophageal reflux and vomiting. The potential for extrinsic acids to erode the teeth is determined by a number of factors including low pH, low salivary flow, and low fluoride content.[iii] This being said, acidic drinks have proved to be particularly harmful when it comes to tooth erosion. As such, clinicians should promote a healthy and balanced diet, with a reduced intake of acidic drinks.[iv]
Chronic trauma from occlusion may occur if abnormal forces are exerted on the tooth for a long period of time. It can cause significant problems for patients, as it leads to progressive changes such as tooth migration, tooth wear, and teeth extrusion.[v] Functional and occlusal issues such as teeth clenching can result in high-pressures being put on the teeth. This pressure on the tooth surface can cause wear, cracks, and fractures.[vi]
The effects of mechanical wear can be made worse by chemical erosion.[vii] This is because acid can either erode the tooth structure directly, or soften the tooth leaving it susceptible to being worn away by hard toothbrushing and/or bruxism.[viii]
The true cost of tooth wear
 In 2022, UK households spent approximately £2.9 billion on dental care.[ix] Tooth wear is common, with the chemical-mechanical process affecting 30% of adults.[x] A 2009 survey of England, Wales and Northern Ireland found that 2% of adults had severe tooth wear (exposing the pulp or secondary dentine), and 15% had moderate wear. This demonstrates the impact that a relatively common condition can have on patients, and the importance of acting early to prevent progression.[xi]
In 2022, UK households spent approximately £2.9 billion on dental care.[ix] Tooth wear is common, with the chemical-mechanical process affecting 30% of adults.[x] A 2009 survey of England, Wales and Northern Ireland found that 2% of adults had severe tooth wear (exposing the pulp or secondary dentine), and 15% had moderate wear. This demonstrates the impact that a relatively common condition can have on patients, and the importance of acting early to prevent progression.[xi]
Not only does dental care impact patients financially, but tooth wear alone can lead to further dental issues. Sensitivity is a frequent complaint from patients with tooth wear, with 60% of patients reporting this symptom.[xii] In severe cases of tooth wear, dental pulp can be exposed, and become infected – this can result in the need for endodontic treatment.[xiii] Other times, although it is becoming less frequently practised, the damage may be so severe that teeth are extracted and replaced with dentures.[xiv] It is important that clinicians have a clear understanding of their patient’s unique anatomy to decide on the best course of action when it comes to restoration, to minimise any further discomfort.
Taking action early to prevent fracture
In order to prevent the worst-case scenario of tooth fracture or loss, pre-empting any issues with occlusion and function which might lead to tooth wear is key. In doing this, clinicians will be able to make the necessary recommendations and provide the treatment needed to improve the patient’s occlusal situation. This might mean offering orthodontic treatment, to align the bite, or a restorative option.
In order to properly monitor a patient’s oral health status, and effectively adjust their occlusion, it’s important to obtain accurate models of their anatomy. This allows clinicians to plan treatment effectively. As digital dentistry continues to evolve, accuracy in this aspect of dental diagnosis and treatment planning is improving. This being said, tools currently on the market, such as intraoral scanners, are not always appropriate for measuring occlusion, as they cannot accurately recreate the bite. As such, until new developments are available for use, analogue dental impression materials are still considered the gold standard for obtaining a highly accurate representation of the patient’s anatomy.
While it is very common, and part of the natural ageing process which comes with wear and tear, tooth wear is an area of concern for many patients. When patients experience significant tooth wear earlier in life, clinicians should investigate the cause and recommend treatments and provide advice to target their specific issue.

https://mimetrik.co.uk

Stephen Claffey Managing Director of Dental Pathway™ and the Independent Dental Advisory Board™
[i] O’Sullivan, Elizabeth. “Tooth wear in children: prevalence, presentation and prevention.” Dental Update 50.10 (2023): 884-889. https://www.dental-update.co.uk/content/paediatric-dentistry/tooth-wear-in-children-prevalence-presentation-and-prevention/
[ii] Gov.uk. Chapter 7: Tooth wear. Accessed February 24. https://www.gov.uk/government/publications/delivering-better-oral-health-an-evidence-based-toolkit-for-prevention/chapter-7-tooth-wear
[iii] Gov.uk. Chapter 7: Tooth wear. Accessed February 24. https://www.gov.uk/government/publications/delivering-better-oral-health-an-evidence-based-toolkit-for-prevention/chapter-7-tooth-wear
[iv] Gov.uk. Chapter 7: Tooth wear. Accessed February 24. https://www.gov.uk/government/publications/delivering-better-oral-health-an-evidence-based-toolkit-for-prevention/chapter-7-tooth-wear
[v] Shetty, Prashanth, et al. “Trauma from Occlusion: Practical Management Guidelines.” Dental Trauma. IntechOpen, 2022. https://www.intechopen.com/chapters/82938
[vi] Uskudar Dental Hospital. What causes tooth fracture? Accessed February 24. https://uskudardishastanesi.com/en/what-causes-tooth-fracture
[vii] O’Sullivan, Elizabeth. “Tooth wear in children: prevalence, presentation and prevention.” Dental Update 50.10 (2023): 884-889. https://www.dental-update.co.uk/content/paediatric-dentistry/tooth-wear-in-children-prevalence-presentation-and-prevention/
[viii] Leeds Teaching Hospitals NHS Trust. Tooth Wear. Accessed February 24. https://flipbooks.leedsth.nhs.uk/LN002840.pdf
[ix] Statista. Annual household expenditure on dental services in the United Kingdom from 2005 to 2022, based on volume. Accessed February 24. https://www.statista.com/statistics/301054/annual-expenditure-on-dental-service-in-the-united-kingdom-uk
[x] Marro, F., Jacquet, W., Martens, L., Keeling, A., Bartlett, D. and O’Toole, S., 2020. Quantifying increased rates of erosive tooth wear progression in the early permanent dentition. Journal of dentistry, 93, p.103282. https://www.sciencedirect.com/science/article/abs/pii/S0300571220300166
[xi] Gov.uk. Chapter 7: Tooth wear. Accessed February 24. https://www.gov.uk/government/publications/delivering-better-oral-health-an-evidence-based-toolkit-for-prevention/chapter-7-tooth-wear
[xii] Gov.uk. Chapter 7: Tooth wear. Accessed February 24. https://www.gov.uk/government/publications/delivering-better-oral-health-an-evidence-based-toolkit-for-prevention/chapter-7-tooth-wear
[xiii] British Society for Restorative Dentistry. Tooth Wear Guidelines for the BSRD. Accessed February 24. https://www.bsrd.org.uk/File.ashx?id=15192
[xiv] British Society for Restorative Dentistry. Tooth Wear Guidelines for the BSRD. Accessed February 24. https://www.bsrd.org.uk/File.ashx?id=15192