The true cost of dental implant treatment
NewsPosted by: Dental Design 1st March 2021
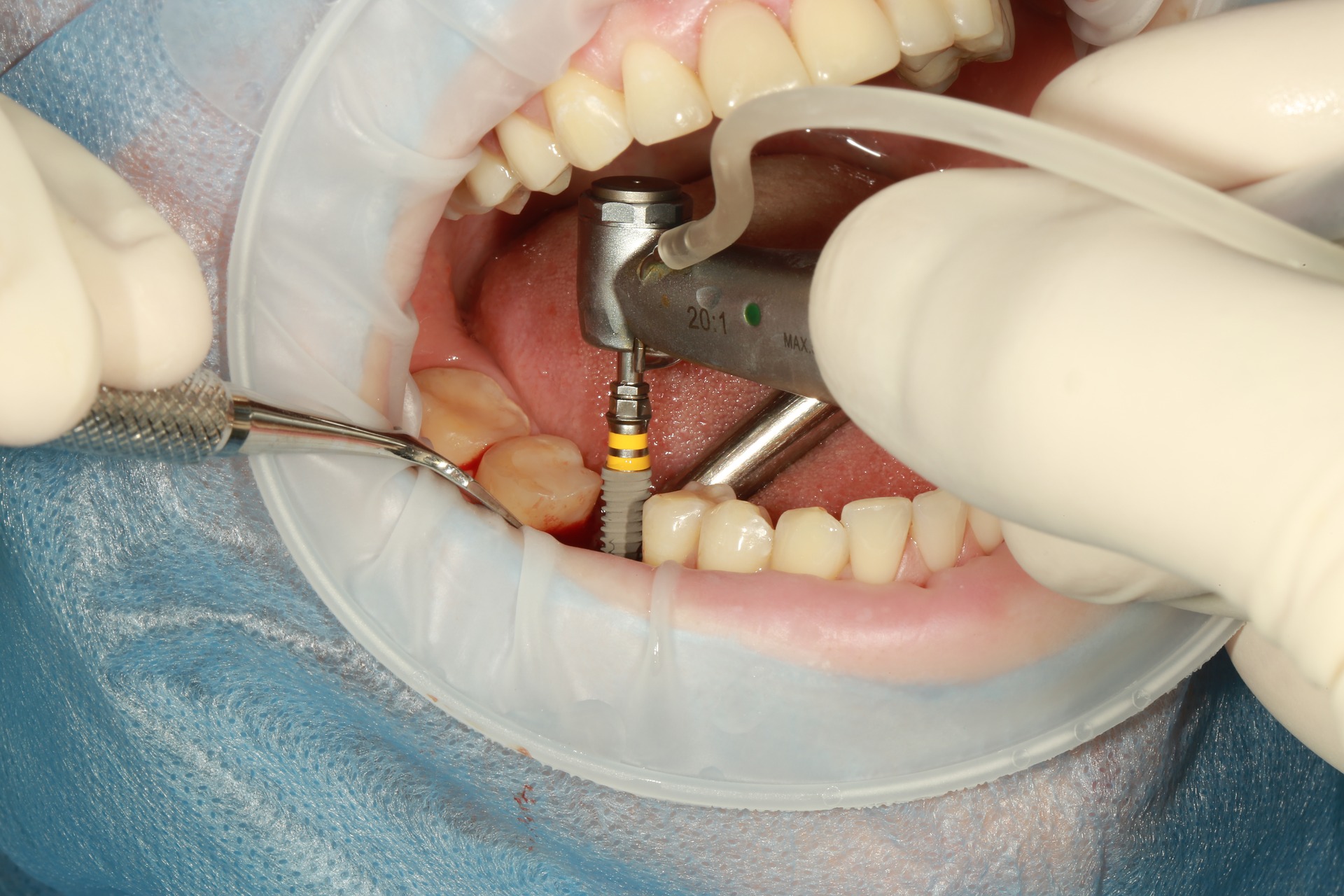
I am sure most of your reception staff have received enquiries like this: ‘’How much does an implant cost?” The Internet is replete with advertisements from providers here and overseas that promise implant treatment at seemingly ‘affordable’ prices. So, can we afford to ‘price match’? How much does implant treatment really cost, to the patient and to you, the provider?
Beyond the obvious outlay that an implant provider must incur such as the costs of intensive training, investment in equipment as well as component and laboratory costs, there are various hidden costs that are not always apparent to such cold callers. When this is met by unrealistic expectations, including the impression that this treatment modality is ‘permanent’, seemingly simple e.g. ‘’just want a smile’’ or ‘’just want a tooth’’ and never in need of regular maintenance or will be trouble-free – the outcome can be disappointing to all parties.
Many of us have also encountered difficult conversations around implant complications from patients who have received ‘affordable’ and complex treatment overseas. These are usually completed over a few treatment visits, where opportunities for corrective actions or a maintenance regime are reduced. With current travel restrictions, any overseas corrective/maintenance trips are now impossible.
The longevity of an integrated fixture and the prosthesis, like that of a well-made and well used car, is dependent on regular servicing and is also subject to wear and tear as well as an array of complications. As such, communicating this to the patient at the outset is prudent.
In terms of complications, the ITI consensus report 2015 vol 8 (Edited by Heitz-Mayfield & Bragger) details a useful classification framework.
Complications can be divided into those that happen peri- & post operative or post-integration. For the former, these are largely preventable with adequately trained operators carrying out treatment in prescribed stages. The use of indexed peri-apical radiograph’s, CBCT, and pre- and intra operative anatomical inspections should render serious haemorrhage, perforation of the lingual cortical plate of the mandible, damage to neighbouring roots/ implants or perforation of maxillary sinus floor and nerve damage, largely avoidable. When an implant is integrated, additional costs can be incurred from complications arising from one of the three categories: aesthetic, biological and hardware related. The latter can be further subdivided into those that relate to mechanical or technical aspects.
The prevalence of such events was reported to be significant in a systematic review by (Pjetursson et al 2014), based on 5-year survival data from 108 studies and different types of implant prostheses. Whilst this is a limited study; it does give us an insight into the potential complexities that implant based restorations can cost. As expected, the incidence of complications for multiple units Fixed Dental Prostheses (FDPs) is greater than that of single units (crowns).
The incidence for full mouth (FM) fixed restorations is even greater. With implant companies and operators advocating FM restorations more frequently in recent years, it is reasonable to expect higher complication rates and related costs in the foreseeable future. The incidence of complications is only part of the story. The other being the degree of complexity in managing such complications. Hence, a chipped porcelain veneer for a screw-retained prosthesis will cost less to repair than that for a cemented one, particularly if it is a multiple unit FDP. Likewise, a loose abutment screw, especially if it’s not frequent, is much easier to deal with than a broken abutment. A damaged framework is expensive to repair but is not as disastrous as broken implants, which fortunately are uncommon events. This may however, become more frequent in the future with increased placement of implants of reduced or narrow diameters (<3.5mm), particularly for patients with parafunction or where increased occlusal load is present.
Whilst the incidence of biologic complications is lower than mechanical complications, preventing and/or managing such problems is an ongoing and long-term process. This is similar to control measures for periodontally involved teeth. The differences are that the cost of maintaining implants has been shown to significantly exceed that for periodontally involved teeth, and the treatment of biologic complications to be less effective (Fardal & Grytten, 2013). In well maintained periodontal patients, increased survival rates and much lower costs of retaining teeth needs to be considered where elective extractions and implant placement is a considered option, especially when long-term maintenance is costed in. Increased susceptibility to periodontal breakdown also increases the risk of peri-implantitis especially if not adequately managed (Karousiss et al 2004; Ferreira et al., 2018). The data related to survival of periodontally involved teeth may however,be biased towards a Tier 2 periodontal setting (Ng et al 2011).
Controlling the cost of implant therapy is therefore similar to all forms of complex dental treatment and encompasses a holistic approach of pre-treatment risk assessment, mitigation measures, and applying an appropriate maintenance regime. Some of the costs are obvious but many are underappreciated and not highlighted often enough. Perhaps the telephone enquiry of ‘’how much is an implant’’ could be compared to ‘’what is the ownership cost of a car of an unknown brand’’ and even more so if bought from overseas? Build quality of the component parts, how they are selected and assembled, driving habits and frequency of use, will all affect the overall cost. Added to that are servicing, regulatory, and insurance costs, one can see the many similarities. Like well-engineered cars that are frequently used, the true long-term cost of implants (and the prosthesis) therefore will not be universally affordable.
There is a tendency amongst the dental community to feel apologetic when implants fail due to biological complications which is not always apparent with teeth. We shoulder all the responsibility when inherent patient related actors are often likely to be the cause. This is especially the case when removal of teeth in the first place was our own recommendation. Implant complications and failures cause increased stress for both the patient and the clinician as well as additional clinical time and costs. If these additional costs are absorbed partially or fully by the clinician, then we need to consider our initial treatment fees. If these costs are to be borne by the patient, then the initial inquiry – ‘How much does an implant cost’ becomes much more difficult to define.
To enquire on our courses, click here – https://perionimplant.com/course-enquiry/
About the authors
Estela Baz.
With Special interest in Periodontology
Having received her Periodontics MCinDent from Eastman Dental Institute, Estela now works at the Perio & Implant DRC, limiting her scope of practice to Implants & Periodontics.
Chong Lim. BDS
(National U. of Singapore) MSc in Periodontics
(Eastman Dental Inst.,UCL), MSc (Distinction) in Dental Implantology (U. of Bristol) Chong heads the Perio & Implant DRC near Richmond Bridge. He is also involved with providing post graduate education for the ITI, Eastman Dental Institute & University of Bristol.










