No strain, no pain
Featured Products Promotional FeaturesPosted by: Dental Design 22nd November 2020

Modern work and leisure patterns have seen a majority of the population now exhibiting musculoskeletal pain. Dentistry is unfortunately one of the most at risk professions, with some reports putting the number of dentists with musculoskeletal pains at over 90%.[i] Even among dentists who’ve been practicing for less than five years, rates of RSI exceed 80%.[ii]
Of course, musculoskeletal strain doesn’t end with work. The rise of smartphones and tablets are encouraging more and more people to look down, or otherwise strain their neck. This can be particularly exaggerated when people use these devices in bed, gradually sliding down until their head is at more than a 45° angle. We naturally tend to orientate our heads with our line of sight over time – look down for long enough and the head will unconsciously follow. Our heads are heavy, on average around 4.5-5kg.[iii] When we tilt our head forward, rather than being balanced on top of the spinal column, the full weight of the head has to be borne by the neck and spine. The greater the tilt, the greater the relative strain. At just 15°, the relative mass of the head increases to 12.25kg, at 30° it rises to over 18kg, at 45° to 22.2kg, and at 60° it is the equivalent of 27.2kg (60 lbs).[iv]
Over time, this strain can have a range of uncomfortable or even debilitating consequences. While the head is bent over, rib movement is restricted, which reduces the efficacy of the heart and lungs. In the short term, the body can respond to the strain by attempting to protect the over-extended spin by forming a fatty deposit at the base of the neck, which is generally regarded as unsightly. Over a longer timescale, poor head posture can contribute to kyphosis, eye strain, and cardiovascular problems. We are seeing increasing numbers of adolescents and young adults with musculoskeletal issues, most likely encouraged by how modern electronics are used.[v]
The aging process is an unavoidable reality, but physical aging is not a consistent process across or even within individuals. Some people are seemingly blessed with youthful looks and vigour well into their middle age, while others look old before their time. Internally as well, some individuals essentially wear out their organs and joints quicker than their contemporaries. Some of this is down to genetics, some due to environmental factors (such as stress), and sometimes our behavioural choices make a difference. For example, someone who drinks excessively is generally going to have a liver that is degraded compared to a person who has not. Under the damage model of aging, we might consider the drinker’s liver to be relatively older.[vi] Repetitive strain induced injuries can be thought of similarly, as a prematurely aging form of damage.
Merely managing pain is not good enough, and there is some debate over the use of NSAIDs (non-steroidal anti-inflammatory drugs) such as ibuprofen, for managing pain from muscle strain injuries. There is some evidence that reducing the inflammatory response can compromise the muscle repair process (particularly in younger patients).[vii] Additionally, long-term reliance on NSAIDs can have adverse effects, including gastrointestinal issues.[viii] What is necessary is to reduce and compensate for damage as soon as possible. Many people only start thinking about these types of injuries once they feel twangs of pain, by which time damage has started to accrue.
 Some evidence suggests that exercise can benefit certain chronic musculoskeletal conditions and pain, and may help prevent some from developing. This does not mean all exercise is helpful – it’s entirely possible to cause further pain and injury through exercising inappropriately.[ix] Constant back pain that gets worse when lying down, or accompanied with weight loss can be a red flag and warrants getting checked for potentially serious conditions.[x] Finding the right exercises depends on the individual’s needs and, ideally, a physiotherapist should be consulted. The NHS provides online recommendations for exercises that can help strengthen and reduce lower back pain, including pelvic tilts and bottom to heel stretches.[xi] There is also increasing awareness of the psychological toll that chronic pain conditions exert. Exercise-based interventions should account for this, and it’s important that physical therapists help build their patient’s trust and confidence.[xii]
Some evidence suggests that exercise can benefit certain chronic musculoskeletal conditions and pain, and may help prevent some from developing. This does not mean all exercise is helpful – it’s entirely possible to cause further pain and injury through exercising inappropriately.[ix] Constant back pain that gets worse when lying down, or accompanied with weight loss can be a red flag and warrants getting checked for potentially serious conditions.[x] Finding the right exercises depends on the individual’s needs and, ideally, a physiotherapist should be consulted. The NHS provides online recommendations for exercises that can help strengthen and reduce lower back pain, including pelvic tilts and bottom to heel stretches.[xi] There is also increasing awareness of the psychological toll that chronic pain conditions exert. Exercise-based interventions should account for this, and it’s important that physical therapists help build their patient’s trust and confidence.[xii]
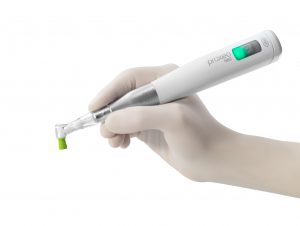
The ergonomics of the dental equipment you use can make a huge difference. Recognised as one of the Product Innovations 2020 in the German Design Awards, the highly ergonomic Proxeo TWIST Cordless from W&H enables you to carry out prophylaxis treatment entirely unrestricted. This handpiece weighs less than many smartphones and is operated via a wireless foot control, minimising unnecessary movement on the part of the user.
Dental professionals are more at risk of musculoskeletal strain than most due to the very nature of dentistry. However, there is a great deal that clinicians can do to mitigate and avoid this problem. Being conscious about your posture in and out of work is the single biggest factor that can help you minimise issues, as can investing in more ergonomic tools and furniture. Finally, appropriate exercises can be of benefit, though care should be taken to research exercises that will help your particular needs, rather than add to your body’s wear and tear.
To find out more visit www.wh.com/en_uk, call 01727 874990 or email office.uk@wh.com
[i] Dias A., da Silva C., Galvão N. Prevalence of repetitive strain injuries/work related musculoskeletal disorders in different specialties of dentists. RGO Rev Gaúch Odontol, Porto Alegre. 2014; 62: 129-136. http://ref.scielo.org/79yjpx March 6, 2020.
[ii] Vyasarayani P., Gundlapalle P., Madhumietha A. Repetitive strain injuries and its incidence in practicing dentists. International Journal of Contemporary Dentistry. 2011; 2(5). https://search.proquest.com/openview/ad67d5a1ef65cdb321420ebfc47fb049 March 6, 2020.
[iii] Gekhman D. Mass of a human head. The Physics Factbook. 2006. https://hypertextbook.com/facts/2006/DmitriyGekhman.shtml March 6, 2020.
[iv] Fares J., Fares M., Fares Y. Musculoskeletal neck pain in children and adolescents: risk factors and complications. Surgical Neurology International. 2017; 8: 72. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5445652/ March 6, 2020.
[v] Fares J., Fares M., Fares Y. Musculoskeletal neck pain in children and adolescents: risk factors and complications. Surgical Neurology International. 2017; 8: 72. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5445652/ March 6, 2020.
[vi] Jin K. Modern biological theories of aging. Aging and Disease. 2010; 1(2): 72-74. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2995895/ March 6, 2020.
[vii] Baker B. An old problem: aging and skeletal-muscle-strain injury. Journal of Sport Rehabilitation. 2017; 26(2): 180-188. https://doi.org/10.1123/jsr.2016-0075 March 6, 2020.
[viii] NHS. NSAIDs. NHS. 2019. https://www.nhs.uk/conditions/nsaids/ March 6, 2020.
[ix] Geneen L., Moore R., Clarke C., Martin D., Colvin L., Smith B. Physical activity and exercise for chronic pain in adults: an overview of Cochrane reviews. Cochrane Library. 2017; 2017(4): CD011279. https://doi.org/10.1002/14651858.CD011279.pub3 March 6, 2020.
[x] Dreisinger T. Exercise in the management of chronic back pain. The Ochsner Journal. 2014; 14(1): 101-107. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3963038/ March 6, 2020.
[xi] NHS. Lower back pain exercises. NHS. 2018. https://www.nhs.uk/live-well/exercise/lower-back-pain-exercises/ March 6, 2020.
[xii] Booth J., Mosely G., Schiltenwolf M., Cashin A., Davies M., Hübscher M. Exercise for chronic musculoskeletal pain: a biopsychosocial approach. Musculoskeletal Care. 2017; 1-9. http://dx.doi.org/10.1002/msc.1191 March 6, 2020.









